What factors have contributed to the rising prevalence of obstructive sleep apnea? There are many factors. Once this is done, patients will have eight hours to sleep and then these sensors will be removed. Some sleep centers have showers so patients may leave the test directly for work if needed. Patients should expect to be at a sleep center for 10 to 11 hours. In addition to completing questionnaires about sleep before and after the study, patients will have sensors applied to their body to measure brain activity, airflow and effort during breathing, heart rate, oxygen levels in the blood, and leg movements. These sensors need to be attached correctly and tested to make sure the signal is high quality. How do these studies work? In-clinic and at-home sleep tests are available, but in-clinic studies, conducted in a specialized sleep laboratory, are considered the gold standard. What are other symptoms? Feeling tired even after a full night’s sleep, morning headaches, mood swings, irritability, insomnia, and waking up with a choking or gasping sensation are among other symptoms.Ī sleep study can measure the number of times a person temporarily stops breathing during sleep. Loud snoring is often a symptom of sleep apnea, but everyone who snores doesn’t have the condition. Brendan Lucey, associate professor of neurology and director of Washington University’s Sleep Medicine Center, explains why the condition is nothing to sleep on. Although snoring might sound innocent enough, sleep apnea carries a range of serious health risks. 
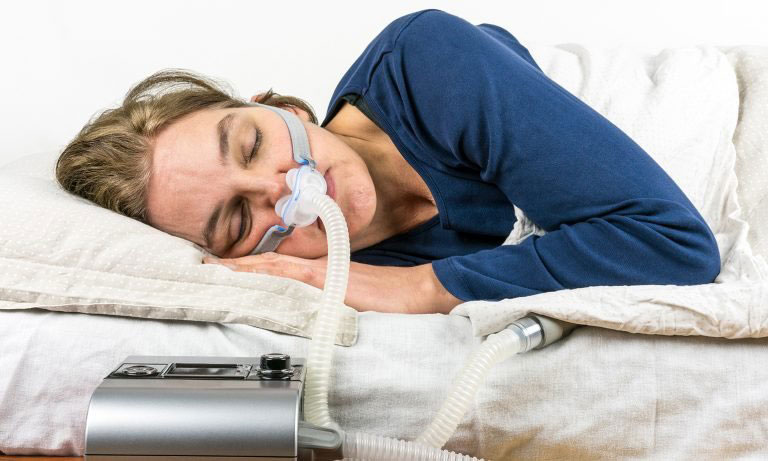
The disorder also affects the quality of a person’s sleep and leads to fatigue during the day. It occurs when the muscles in a patient’s airway relax and obstruct the passage of air, causing the person to snore loudly and abruptly wake over the course of the night. Obstructive sleep apnea, a condition that causes breathing to stop and start throughout the night, affects millions of Americans. But for some, feeling refreshed upon waking up is no guarantee. Highly trained staff are also available to consult with investigators in the use of these methods.įor service availability, costs, and general operating procedures of the lab, and to include lab services in a research proposal, please contact the Office of Nursing Research at more about our Center for Innovation in Sleep Self-Management.It’s hard to beat a good night’s sleep. We also maintain a library of rigorous protocols for sleep actigraphy data collection, cleaning and analysis polysomnography data collection and analysis and physical activity actigraphy data collection, cleaning and analysis. The sleep lab also has the expertise to help investigators make, repair, and recondition small laboratory equipment.Software is available for scoring the activity data for sleep detection and cosinor analysis of temperature data.Numerous microprocessors (Mini-Mitter® actigraphy) are available for recording of activity and body temperature (BioPac).A portable computer-based polysomnographic sleep recording system is available for monitoring sleep in home or clinic settings.Polysomnographic recordings of sleep can be obtained from three subjects simultaneously by means of a computer-based sleep EMBLA acquisition system.The laboratory bedrooms are fully equipped to accommodate both pediatric and adult research participants. Our fully equipped UW School of Nursing Sleep Research Laboratory consists of a control room, a sleep study research area with three bedrooms, and shower/bathroom facilities. Read about the School’s rich history of sleep research. The UW School of Nursing was the first nursing school in the United States to launch a fully functioning sleep research laboratory. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
